
Belinda Hatfield (Photo: David Berman/Gazette)
One of the greatest concerns of our breast cancer patients is the development and prevention of lymphedema. Approximately 5-10% of patients who have undergone radiation treatment and axillary lymph node dissection will develop lymphedema in their arms. The average time to develop these symptoms is about 18 months after the completion of radiation treatment.
Fortunately, there have been recent advances in understanding the causes and mechanisms of action of this condition. Read on to learn more about the present and future of lymphedema therapy.
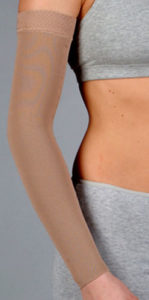
Compression Sleeves (Photo: lymphedemaproducts.com)
The Compression Sleeve
The primary lymphedema treatment is manual decongestive therapy. By wearing a compression sleeve or using a lymphedema pump, patients can control their symptoms by reducing the amount of lymphatic fluid in their affected limbs. Many patients dislike compressive garments because they can be uncomfortable, hard to cover up, and often limit everyday activities.
On the other hand, lymphedema pumps need to be used daily and might be expensive to purchase and replace.
Vascularized Lymph Node Transfer Technique
Two recent developments in lymphedema surgery have shown promise. The first technique is the “Vascularized Lymph Node Transfer”, which removes the healthy lymph nodes from one area of the body and transfers it to where the patient had the initial lymph node removal.
Common donor sites for Vascularized Lymph Node Transfer are the lower abdomen and the chest. We must be mindful to prevent lymphedema from occurring in the donor sites. Often, we can transfer lymph nodes at the time of the DIEP flap. In this case, there is no additional surgery nor recovery time apart from the breast reconstructive operation.
This procedure allows us to remove any scarring that may be preventing the flow of lymphatic fluids. It also provides a long term solution in the areas affected by lymphedema.

Belinda Hatfield (Photo: David Berman/Gazette)
One of our patients, Belinda Hatfield, recently described her experience with this surgery.
(Read her story to learn more about this procedure)
The second operation is the “Lymphovenous Bypass.” Using microsurgery techniques, the surgeon can reroute a patient’s lymphatic channels into blood vessels that will also allow for a reduction of lymphedema fluid. This procedure can be done in an outpatient setting through small incisions on the arm to locate the lymph vessels and venous systems.
Although both of these surgical treatments are under active investigation, they offer hope in improving the quality of life of patients with lymphedema.

One thought on “Vascularized Lymph Node Transfer (VLNT) for Lymphedema”
Dear Dr. Tiwari,
I just read your article on Vascularized Lymph Node Transfer and I’m very interested. I have edema on my chest an underarm and sometimes on my upper arm. I also have neuropathic pain from the lymph node dissection. I have been talking with Dr. Corinne Becker in Paris France and I’ve been examined by her when she was in the US recently. I live in KY but I am considering going to Paris for the VLNT procedure. Ithis procedure? I would like to discuss this further with you. didn’t realize anyone in this area was doing the VLNT. Would you be available to talk with me more about
Thanks so much for your time.
Kim Thomas