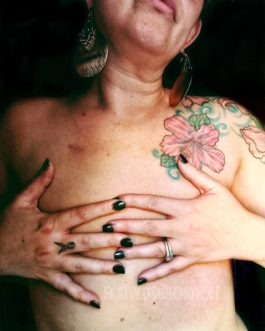
Emily Hopper’s gallery photo from Flat Closure Now.
In our practice, we see an increasing number of patients who have undergone prior mastectomy and have chosen to forgo any breast reconstruction procedures. Unfortunately, these patients are oftentimes left with excess skin and soft-tissue at the inframammary fold area – the lateral trunk area – and sometimes overhanging their mastectomy incision. Many of these patients have been quite clear and explicit in their desire not to undergo reconstructive surgery.
Tragically, some of these patients nonetheless were left with excess skin to allow for potential future reconstruction. This type of flat denial medical course is one that we, as surgeons, must re-evaluate.
[pms type=”gallery” option=”page” procedure=”flat-closure” sticky_only=”0″ with_sticky=”1″]
Flat Result Techniques
One of the primary concerns for patients is that their wishes to remain flat after mastectomy be respected. From a surgeon’s perspective, achieving an aesthetic and normal contoured flat result can be quite difficult. Many breast surgeons, who are general surgeons by training, may not be familiar with certain plastic surgery techniques such as standing cone deformity excision, local transposition flaps, and fat grafting to address contour deformity areas, Pectus excavatum, and asymmetries of the chest wall. As such, achieving a truly flat result can be a difficult outcome to achieve.
In our practice, we have developed a process for effective communication with our breast surgeons to address patients’ concerns who desire to remain flat. We have a combined approach to achieve this desired result. In developing such a program, we have realized that many patients would like to proceed with a “one-and-done” type result after mastectomy to achieve a flat result.
Realigning with Patient Expectations
In my opinion and our experience, I believe that we, as surgeons, must work to realign patient expectations. I think that promising a single-stage aesthetic flat result is, more often than not, an unreasonable level of expectation to set for patients.
I meet with many patients who have expressed a desire to be flat after mastectomy. These meetings can be before mastectomy surgery or after they have healed from a mastectomy. During this conversation, we discuss the specific issues that I will foresee for them.
As a reconstructive plastic surgeon and microsurgeon, I must take into account variables such as:
- Body mass index
- Native breast volume
- Soft tissue properties
- Breast size
- Tumor location
- Need for radiation treatment
In our practice, we are oftentimes successful with insurance coverage for these types of reconstructive procedures under the auspices of the Women’s Healthcare Act of 1998.
Allowing a Consistent Result
It is important to understand that addressing the patient’s anatomical constraints and explaining what they will expect after a mastectomy is critically important to set the appropriate expectation level.
In our practice, the optimal time to achieving an aesthetic, flat result is approximately three months after mastectomy. This time frame allows for adequate healing and soft tissue softening to achieve a truly flat result.
Plastic surgery techniques such as total en-bloc capsulectomy, implant removal, excision of standing cone deformity, local transposition flaps, and fat grafting are tools in the plastic surgery toolbox to allow for a consistent result.
High-quality Outcomes for Patients
For many patients achieving an aesthetic flat result allows a significant measure of control over the decision-making process, allows for patient empowerment, and allows wearing an external prosthesis appropriately if they so choose. The surgical community has much work to do to improve surgeon education and patient communication on this important topic.
Plastic surgery is a science built on delivering results that meet the patient’s expectations, and we must be careful to avoid a one-size-fits-all approach.
As the flat closure community continues to develop, there is a great opportunity to develop approaches that safely deliver high-quality outcomes to our patients.

10 thoughts on “Going Flat After Mastectomy”
The focus of this article is for an aesthetically pleasing result for women who desire to go flat.
I looked at your online gallery, and I do not see any photos showing the before or after of staying flat
Hi Carmen. We have recently uploaded a photo of one of our patients who agreed to allow us to publish her before and after photos going flat here: https://mwbreast.com/gallery/
How can I find the best plastic surgeon for a REVISION of a horribly done explant in the Miami, Florida area?
I was wanting to go to Dr. Rankin in Jupiter Florida and he had a very long waiting list. I live in Ohio and was going to stay in Jupiter with a friend who lives there. I am so very grateful to Midwest Breast as Dr. Kocak did a wonderful job. I got my explant surgery in about two months after my consult. I was so sick with my implants which I had for 11 yrs after dmx due to breast cancer. I’m so much healthier now and credit them with saving my life!! I’m flat and happy! I’m in the before and after pics. Age 50-59 on the first page of this article. Hope this helps someone. 💕
this is a great article and i hope many see it. I had subpectoral implants after my dmx 13 years ago and wish very much i had known about the discomfort and unattractive contours, and had a knowlegeable surgeon. The one I had told me if I ever wanted them out, he ‘didnt know what your chest would look like’. I hope he knows more now. Very few doctors have as much knowledge as you show in this piece. I wonder if you know of any surgeons who could do a good flat closure in the New York City area , where I live. Thank you.
Replying to my own comment as this is not answered, maybe outside doctors boundaries to say. Should be noted that Not putting on a shirt and Flat closure now have advocacy groups and I hope to be able to add names to their rather short lists in time. Their Facebook discussion groups have a number of women who have had good results and name their doctors.
I love those groups too but this is where I found my amazing surgeon. They list explant surgeons by state. Only the good ones that the members refer. I refer Dr.Kocak to everyone who will listen.
https://www.healingbreastimplantillness.com/
I have the misfortune of going to an educational hospital (medicaid) and although I only had DCIS, no radiation, no chemotherapy – I got a bilateral mastectomy with no reconstruction due to family history and risk levels. I have a small torso, was in great shape (it was the prime of my life, in my 30s), only size B — absolutely NO obstacles to getting a good result on my end or situation. One side of my chest is near perfect, clearly done by an expert. The other side – done by a “breast fellow” (general surgeon at the beginning of their breast surgery specialty). Letting this person touch me is one of the biggest regrets of my life. The results are so irregular, I had a seroma where they took too much tissue, it goes in too far in one area, I have stitch marks still 4 years later, and my surgeon left behind all the tissue underneath my scar. So I am stuck with a half moon of fat hanging off the middle of my chest for no reason – except for a surgeon’s lack of skill. And this was my healthy, prophylactic side. They only give me access to unskilled plastic surgeons to revise it. This has made the whole process 100x harder and more depressing than it should have been. The skin on that side clashes when I move. My hospital valued giving doctors experience more than my outcome/life. My chest still looks better than 85% of pictures I see (and I did my part to have realistic expectations) but this left behind bump of fat bothers me daily and fills me with anger. More doctors should realize how important good cosmetic results are even for women who choose not to get reconstruction. My surgeon gets to move on with their life while I’m stuck with their terrible work and no help to fix it. Life is incredibly unfair.
I don’t know where you are located but this website has a long list of experienced explant surgeons listed by state. That’s how I found this amazing place.
https://www.healingbreastimplantillness.com/
if a woman goes flat, no surgeon should ever ask her “do you want implants” years later. It’s annoying. If someone wants them, they will get them initially, or ASK. Stop asking me if I want this crap in my body, I don’t. Doctors (especially female doctors) can be so careless about this.